The Health Virtuous Circle
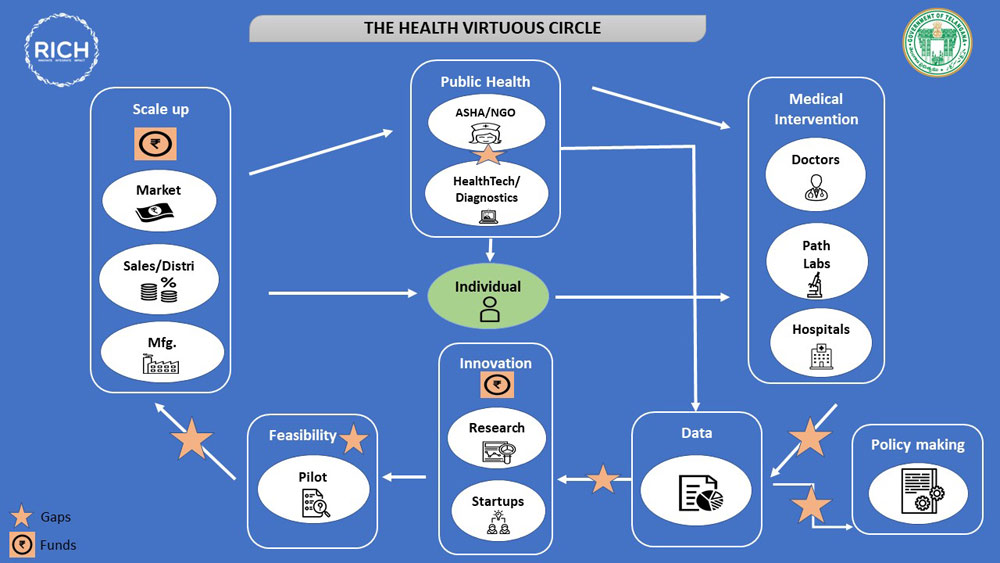
Global spending on healthcare is projected to increase from US $9.7 trillion in 2015 to US $18.28 trillion by 2040 with a projected worldwide shortage of 12.9 million healthcare professionals by 2035.
Increasing demand for health services and escalating healthcare costs are pushing governments to improve access and quality of care. These trends are likely to steer the short-term and the long-term healthcare strategies.
Certain components of the health systems the world over are common, even as the levels and pace of implementation differ across countries. Universal components include regulators, payers, infrastructure, consumer engagement and innovation.
One of the major policy initiatives of the Indian government has been the announcement of Ayushman Bharat – Pradhan Mantri Jan Arogya Yojana (AB-PMJAY), a health insurance scheme for the economically weaker section of the Indian population. This initiative, if implemented effectively, will help the nation move closer to the Sustainable Development Goal of ‘Universal Health Coverage’. The scheme aims to cover nearly 55 crore beneficiaries from over 10.74 crore deprived families as per socio-economic and caste census (SECC) data with an annual health cover of INR 5 lakh per family per year taking care of almost all secondary care and most tertiary care procedures.
AB-PMJAY envisages the adoption of standardized treatment protocols, pre-defined costs for secondary and tertiary procedures, and use of IT and data analytics for seamless implementation and prevention of fraudulent claims. The scheme is expected to generate enormous volumes of data that could be used for studying the disease-demography links, which in turn could help in developing better and targeted public health programs.
While multiple State government-sponsored insurance schemes exist in India, the overall penetration is still relatively low. These schemes are fragmented and each offer a different benefit package. More than 2/3rd of the expenditure (~68%) on healthcare is out-of-pocket. Also, current health insurance covers in-patient treatment and mostly excludes OPD/medicines/diagnostics. The execution of the scheme, therefore, will be a big challenge since it would involve identifying the critical success factors, allocating the required monetary support, incentivising the stakeholders and acting speedily to cover all the beneficiaries.
Effective treatment begins with accurate diagnosis and to achieve this goal, the hurdles of costs and reach need to be tackled. India’s extensive dependence on import for medical devices (about 80 percent) poses a big challenge for affordability. The demand isn’t just for the traditional high-end equipment but also for newer point-of-care devices. Preventive healthcare can reduce costs, which creates even greater incentive to bring newer devices and diagnostics to the market faster. New healthtech devices allow individuals to monitor their health on a regular basis. Increasing awareness coupled with virtual tools has started to bring a major shift in the health management business. Although several health-monitoring products are available, there exists a lot of ambiguity with respect to their use due to lack of regulatory guidance. This results in a lot of lost opportunities to connect digital health with conventional health systems. In order to fully harness the opportunity, the industry needs strategies to boost resources to utilize technology to manufacture such devices with ease, speed, and compliance. Initiatives like ‘Make in India’ can help bridge this gap.
The efforts of creating infrastructure and service delivery would be incomplete without factoring-in access to newer medical technologies. It is extremely crucial to empower the community healthcare workers with technology and the required skills if last mile delivery is to be successfully achieved. The increasing use of new diagnostics and devices has created a huge gap in the skill levels of the healthcare workers. The MedTech sector has a vital role to play in ensuring availability and affordability of medical devices for the masses, which will prove to be one of the critical contributors to the long-term success of the scheme. The industry can also contribute by providing training to healthcare professionals and making them technology-ready.
It is common knowledge that most of the innovations and technology breakthroughs get limited to individuals and hospitals in cities. Due to lack of accessibility, infrastructure, affordability and trained medical professionals, rural healthcare still remains a challenge.
To tackle this challenge, a large number of startups are offering solutions in the form of mobile apps, point of care devices, mobile diagnostic vans for screening of rural population. In Hyderabad alone, there are numerous startups working in the areas of integrated healthcare management, artificial intelligence, machine learning, non-invasive testing, electronic health records etc. with an aim to cater to the rural population and create an impact on the overall public health.
On the one hand there are organizations like Piramal Swasthya, which have been working in the rural sector for years and have wide reach in terms of locations and access, and on the other hand, there are startups such as Nanohealth, Docturnal and Medic, which are new and require patient data for validation. Nanohealth, for e.g., deals with healthcare management program, Docturnal claims to use a device which can detect TB through cough, Medic uses a mobile app in a local language for doctor visits, diagnostic tests etc. All these startups are more or less targeting the same population for the testing of their products. To maximize the efforts of these new startups, and to leverage the reach and experience of the older organizations like Piramal Swasthya, RICH (Research and Innovation Circle of Hyderabad) is connecting such players with each other so that they can explore ways in which each can benefit from the other. RICH also plans to bring together all such players in this sector on a common platform so that they can figure out ways to collaborate with each other.
Although the healthcare startups are making serious inroads in the diagnostics and wearable devices space with new age technology, these startups face funding crunch at the pilot stage. Several government schemes are available for very-early stage funding, which fizzles out once the startup is ready for the next step. New technology has great potential to provide a platform for disruptive innovation, which can create out-of-the box, innovative and cost-effective solutions for the masses. Serious gaps also exist when it comes to scaling-up of innovations. Unfortunately, these gaps are not just limited to funding. Lack of knowledge about the avenues available for market access, intellectual property protection, prototype building, testing, validation, availability of equipment, large scale manufacturing etc. is common. Thus, in the interest of promoting indigenous solutions and domestic manufacturing, startups need to be supported by providing funding and mentoring.
As more and more people and organizations rely on mobile devices, social media channels and big data for everything related to their work, health and social life, data privacy has attracted enormous attention. There is a huge volume of personal information about every individual stored on various computers and in the cloud and exchanged every day. Consequently, there is a heightened concern about ways in which that information could possibly be used. Recent cases of data breaches also add to the worries. While individuals prefer to protect their personal information, especially medical records, this data is a vital component in advancement of healthcare. Comprehensive information from diverse population can help accelerate research and policy making. In the current scenario, the challenge is to create awareness about the need of researchers and policy makers to have access to personal health data, while also ensuring availability of technologies and processes to protect that data.
Ministry of Health and Family Welfare’s (MoHFW) draft legislation called Digital Information Security in Healthcare Act (DISHA) is a step in that direction. DISHA aims to regulate the collection, storage, use and transmission of digital health data and provides for data privacy, confidentiality, security and standardization. The vital step is to create right policies to safeguard the information and to ensure their continued implementation so that while the data is kept private, it is also shared in a useful way.
As part of adoption of digital strategies, lifesciences companies will benefit immensely from collaborations with technology companies. Technology partnerships can open up new opportunities in healthcare across various domains. We are already beginning to witness a shift from traditional alliances to a more collaborative approach to partnerships. This approach often involves various ecosystem stakeholders such as industry, academia, researchers, startups, entrepreneurs and government.
With the country offering numerous competitive advantages in terms of R&D facilities, knowledge, skills, and cost effectiveness, the healthcare industry in India has immense potential to emerge as a global key player. Having said that, we need to ensure that the fruits of this progress are enjoyed by not just a certain section of society, but by the ones who are most likely to be left behind.
https://www.pwc.com/gx/en/healthcare/pdf/global-top-health-industry-issues-2018-pwc.pdf
https://www.pwc.in/assets/pdfs/publications/2018/ayushman-bharat-national-health-protection-mission.pdf
https://www.medicalbuyer.co.in/make-in-india-can-pave-the-way-for-successful-implementation-of-the-ayushman-bharat/
https://www.medicalbuyer.co.in/the-keystone-for-ayushman-bharat/
https://health.economictimes.indiatimes.com/news/industry/disha-to-give-direction-to-digital-information-security-in-healthcare-supratim-chakraborty/63993563
https://health.economictimes.indiatimes.com/news/industry/disha-to-give-direction-to-digital-information-security-in-healthcare-supratim-chakraborty/63993563
https://www.nhp.gov.in/NHPfiles/R_4179_1521627488625_0.pdf





